They are in turn rated by a group of medical experts; results were disappointing for them as it appears below, and no system could earn an “A” grade:
- US NEWS earned an overall B
- Hospital Compare (CMS) a C
- Leapfrog received a C-
- Healthgrades got a non-passing grade of D+
More disturbingly, they too often provided conflicting information on the rating attributed to the same hospitals. We hence propose to take a closer look at the different methods used to rank hospitals and try to give the reader advice on how to run their research, using these and other possible tools.
To do so, we mainly analyzed the NEJM “rating the raters” study to discriminate between these methods and select the right criteria to use them.
Our recommendations
Primarily go to the US NEWS ranking, based on the following findings
- It includes a reputation criterion, from surveys of practicing providers in 16 specialties, answering the question “where would you send your most challenging cases?”. Respondents can select up to five hospitals, including their own.
- Another very important factor is volume as a quality measure, which none of the other rating systems include. We believe this dimension to be essential since it provides a quantifiable measure of:
– Regular team practice, which is a key factor in the quality and safety (1) of a medical team,
– Reputation, as perceived by patients, as opposed to the potentially biased physicians’ assessment of their peers - Finally, assessing quality at the specialty level makes much more sense than following it globally: in each hospital, not all the teams are at the same level of quality, safety and competence.
(1) in France, for example, hospitals that do not perform a sufficient number of a given surgery, are no longer authorized to practice it, due to proven security concerns.
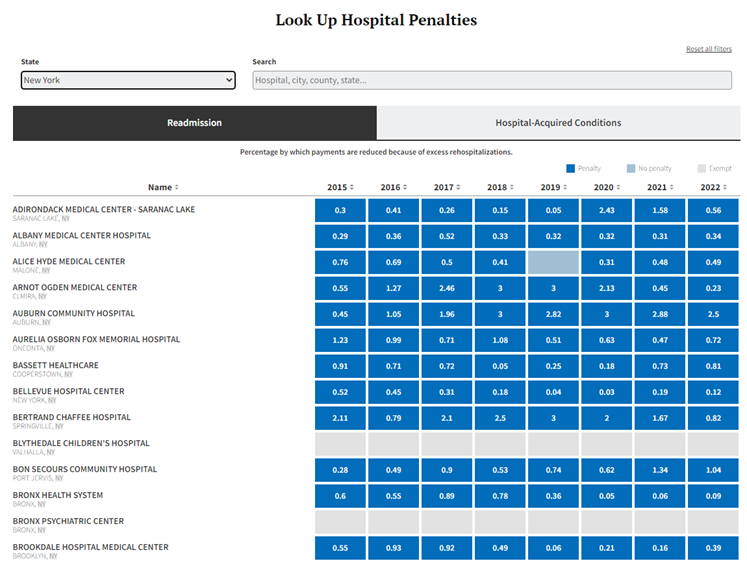
Look at the CMS’s HRRP results
HRRP, the Hospital Readmissions Reduction Program was created by the 2010 Affordable Care Act and began in October 2012 as an effort to make hospitals pay more attention to patients after they leave. Readmissions, measured within 30 days after discharge, occurred, and are still occurring, with regularity.
2 main reasons to use readmission rates:- It is very selective: of the 3046 hospitals included in the program in 2021, only 247 (18%!) received no penalty
- Unlike other CMS measures, HRRP readmission rates are risk adjusted to account for the incoming health of a patient. The sicker a patient is upon their first hospital admission, the greater the likelihood he/she will be readmitted. It therefore avoids the criticism that teaching hospitals have difficulty achieving a 5-star rating because they generally treat the riskiest cases.
KHN (Kaiser Health News) provides the comprehensive dataset including all hospitals in the country through a look-up tool.
In the same page, another tab gives the patient safety penalties on Hospital acquired conditions.
Finally, we recommend patients to also to take the advice from their doctor and to discuss this with their trusted family circle.





